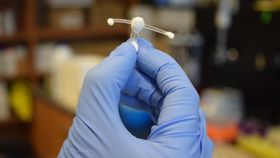
A team of Canadian and Kenyan scientists has developed a vaginal implant that could help prevent HIV infection in women by suppressing the responsiveness of immune cells in the female genital tract.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.An experiment summarized in the latest issue of the Journal of Controlled Release showed that the flexible polymer device successfully induces a prolonged state of “immune quiescence” in rabbits by slowly releasing an anti-inflammatory drug called hydroxychloroquine. If subsequent trials prove effective, the simple, low-cost invention could assist in reducing the spread of HIV among the world’s most vulnerable populations.
HIV can only replicate in the human body after it attaches to the surface of one of several types of white blood cells – or lymphocytes – whose purpose is to detect and destroy pathogens. Thus, although it may sound counter-intuitive, inhibiting the immune system’s reaction against viral particles present in the female genital tract actually interferes with the virus’s ability to gain its initial foothold in the body.
The virus has a particular affinity for a type of lymphocyte called a T cell. When T cells are activated, they secrete inflammatory molecules that recruit more T cells and other immune cells to defend against whatever invader first tripped the alarm. When the body’s T cells show low levels of activation, but the immune system is still functioning correctly, one is said to be in a state of immune quiescence.

Two of the study’s researchers, Emmanuel Ho and Keith Fowke, had previously studied a group of Kenyan sex workers who displayed puzzling immunity against HIV despite having sex with HIV-positive clients. Ho and Fowke eventually determined that these women were protected because of their naturally quiescent T cells.
"Observing this, we asked ourselves if it was possible to pharmacologically induce immune quiescence with medication that was better assured of reaching the point of infection," said Ho in a statement. "By delivering the medication exactly where it's needed, we hoped to increase the chances of inducing immune quiescence."
Hydroxychloroquine, a microbicide that was first developed to treat malaria, was selected due to its recently discovered ability to inhibit a type of cell surface protein necessary for T cell activation.
According to Ho, the team has yet to determine whether the device is effective enough to be used as a stand-alone, or if it is better suited as a backup method – alongside safe sex practices and anti-viral medications – for women at high risk of infection. How long each implant can last also remains unknown.
“We aim to answer these questions with future research," said Ho.
Following decades of public health campaigns and clinical outreach, HIV transmission rates have declined in developed nations in recent years, yet the threat of HIV and AIDS remains very real in low-income areas. Eastern and southern Africa account for approximately 70 percent of the world’s current HIV infections and 43 percent of the global total of new HIV infections occurring yearly.
Woman and girls are disproportionately affected by the epidemic due to lack of access to prophylactic medications and an inability to protect themselves against exposure from male sexual partners who have sex with multiple other partners without protection.