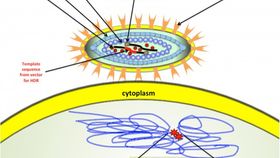
The virus that causes AIDS has been altered so that it can change the human genome in ways that could improve and extend the lives of people with a multiplicity of diseases - including HIV itself.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Scientists have been conducting experiments on the use of viruses for gene therapy since the late 1990s. Natural selection has been honing the capacity of viruses to work their way into cells for millions of years. If we can take advantage of that capacity to deliver beneficial genes the potential uses for medicine could be endless.
Not all viruses are equally suited to this task. The immune system recognizes many viruses and attacks them. Other potential carriers are genetically unstable, making them unsuitable to the task. Naturally it is also essential that any virus used is either harmless, or has been modified to make it so.
In eLIFE three medical researchers from Aarhus University, Denmark, describe “adapting lentiviral vectors as carriers of designer nuclease proteins, providing efficient targeted gene disruption in vector-treated cell lines and primary cells.”
Enzymes developed by microorganisms to slice viral DNA have been used as so called scissors in gene therapy, but the targeting has improved in recent years with the creation of hybrid enzymes.
"Now we can simultaneously cut out the part of the genome that is broken in sick cells, and patch the gap that arises in the genetic information which we have removed from the genome. The new aspect here is that we can bring the scissors and the patch together in the HIV particles in a fashion that no one else has done before," says author associate Professor Jacob Giehm Mikkelsen.
While the safety issues involved in using viruses are obvious, gene therapy usually involves a more hidden danger. "In the past, the gene for the scissors has been transferred to the cells, which is dangerous because the cell keeps on producing scissors which can start cutting uncontrollably,” says Mikkelsen. "But because we make the scissors in the form of a protein, they only cut for a few hours, after which they are broken down.”
Meanwhile, the team's virus brings along the genetic material required to patch the hole. “"We call this a 'hit-and-run' technique because the process is fast and leaves no traces,” says Mikkelsen.
The Danish team are not the first to use HIV as their delivery vehicle, but they sliced the virus' DNA into shorter sections and fused these to sequences for making the hybrid enzymes to produce the “fusion proteins”. This approach gives much greater control over the changes wrought to cells' DNA.
Not only could cells be changed to cure hereditary diseases, they could be dosed with genes suited to fighting cancers. There has even been work on having cells produce anti-viral proteins, so that one day modified HIV might bring be used to bring genetic sequences that protect against HIV itself.
When applying the technique to cultured cells the Micckelsen and his colleagues found 20% were successfully edited. While one in five is far from ideal, Professor Perry Hackett of the University of Minnesota commented in the same edition of eLIFE that this “approaches the levels required for effective gene therapy in whole animals—including humans.” Further work may raise the success rate, although application to living creatures is still yet to be demonstrated.