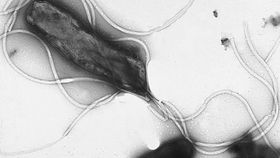
When the bacterium Helicobater pylori, the cause of stomach ulcers, first infects a new host it engages in an exceptional bout of evolution in order to evade the immune system, a paper in Nature Communications reveals.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.H pylori was already known to be a remarkable microbe, with early reports of its existence dismissed before confirmation led to its discoverers winning the Nobel Prize. The initial skepticism was based on the fact that the acidic environment of the stomach makes for an exceptionally hostile environment, one in which most bacteria cannot survive for long.
Professor Stephan Schuster led a team at Penn State that collaborated with H pylori co-discoverer Barry Marshall to study the bacteria's genome for two strains in both humans and rhesus macaques. The volunteers were people who had asymptomatic infections and were willing to go through a treatment with antibiotics before being deliberately re-infected (rather like Marshall himself), allowing the team to study the bacteria's DNA both before infection and at several points thereafter. "Our next-generation sequencing approach enabled, for the first time, the tracing of Helicobacter pylori infections in human patients," Schuster said.
"We were blown away by the very high mutation rate that we found during the initial phase of infection," said lead author Dr Bobo Linz. "We found that the bacteria accumulated mutations at a rate 30 to 50 times faster during this acute phase than during the later, chronic phase of infection when an equilibrium was reached between the bacteria and the immune response.”
Chronic phase mutations had been measured before, but the rate of evolution in the acute phase had not been anticipated. Nevertheless an explanation is apparent. H pylori infection causes the immune system to release reactive molecules that break up chromosomes and induce changes to DNA.
"Strains of the bacterium isolated from different human hosts vary immensely, both in DNA sequence and in gene content" Schuster said. "There are about 1,100 core genes that individual strains of H. pylori share, but another four-to-five-hundred genes vary between strains. The high mutation and recombination rates that produce this variation allow the bacteria to be exquisitely adapted to its host and to evade eradication by the host's immune system."
The immune system targets proteins on the surface of pathogens. Linz noted, "Antibodies are so tuned to recognize the three-dimensional structure of outer-membrane proteins that they can attach to them with lock-and-key specificity, thereby labeling the foreign bacteria cell for elimination.” Changing surface proteins allows diseases to escape the immune system. However, this is normally done through different strains of the disease swapping genes to produce a new version.
However, for H pylori the reactive molecules have a similar effect. "The intense selective pressure on the bacteria to survive the immune response, coupled with increased mutation rates, produces the incredibly fast rate of genomic change that we discovered in this study," said Linz. "Mutations occur randomly throughout the genome, but because they help the bacteria avoid elimination by the immune system, changes in outer-membrane proteins appear much more often than would be expected by chance in the surviving bacteria."
The researchers intend to see if bacteria infecting other parts of the body also evolve rapidly in response to pressure from the immune system. Meanwhile creationists will be over in the corner pretending none of this is happening.