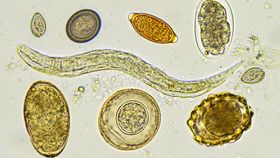
Helminth therapy is a new frontier in experimental medicine, promising to cure all manner of conditions from allergies to autoimmune diseases to irritable bowel syndrome to even, possibly, autism.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Here’s the catch: It is not yet recommended or approved by the FDA and there is very little interest in the treatment from members of the established medical community. This means anyone wanting to try it out for themselves will have to sign onto a clinical trial (which are sporadic and small in number), travel abroad, or look to the grey market and the unregulated, often unscrupulous companies offering helminth therapy online.
So what does this encouraging – if deeply controversial – therapy actually involve?
The short answer: intestinal worms.
Patients purposefully inject or ingest intestinal worms (aka helminths) or their larvae to reboot their immune system and calm symptoms of inflammation-related conditions. The theory goes that, in order to survive inside a human host, a helminth must regulate the body’s immune response and, by doing so, prevent it from overreacting to internal and external stimuli – the physical process behind autoimmune diseases.
It sounds icky. After all, most of us have been brought up to think of intestinal worms as parasites and a harbinger of disease, sickness, and, in some cases, death. Yes, contracting worms can trigger a range of unpleasant symptoms, including diarrhea, abdominal pain, malnutrition, and fatigue. It can also impair growth and physical development in children, and in the worst case scenarios be life-threatening. Yet, the right type of helminth in the right quantities may be beneficial to its host – and perfectly safe.
“Helminths are a lot like bacteria,” William Parker from Duke University’s Department of Surgery told IFLScience. “Some of them can kill you and some of them are beneficial.”
Helminth advocates like Parker refer to the “Old Friend Hypothesis”, which postulates humanity has spent the majority of its existence living alongside benign microbes – and that includes non-harmful parasites and helminths. We’ve co-evolved over tens of thousands of years. In essence, we and they are “old friends”.

Only recently, following the economic prosperity and technological boom kick-started by the industrial revolution, we have lost our old friends. Modern society is too clean. At least, it is in the West. More than 1.5 billion people worldwide are infected by soil-transmitted helminths, the majority in sub-Saharan Africa, the Americas, China, and East Asia, and when worm eradication programs do take place, studies show that rates of autoimmune diseases spike in the immediate aftermath.
“[Helminths] are a natural part of our environment that we’ve lost and they really need to be put back into everyone for disease prevention, we believe, not just for disease treatment,” said Parker.
Parker, who has spent years studying intestinal worms’ effect on the human immune system, sees helminths as a therapy rather than a drug. He argues we will need to “reconstitute our biomes” by re-introducing helminths to our body’s natural eco-system.
“We’ve essentially annihilated them all from our bodies, from our own eco-systems,” he added. “Whenever you disturb an ecosystem, sometimes it doesn’t do what it’s supposed to do.”
While it may be that we can all benefit a little from an intestinal worm or two, the people who are likely to benefit most are those with inflammatory health issues – particularly those with an autoimmune disease like lupus, celiac disease, and multiple sclerosis (MS). It could also be used in treatments for digestive disorders like irritable bowel syndrome (IBS), neuropsychiatric disorders like anxiety and depression, allergies, and migraines. Some studies even point to helminth therapy as a possible avenue for people with autism: Autistic adults were more adaptable and less likely to perform repetitive actions following a 12-week program involving whipworm eggs.
“The science is very solid,” explained Parker. “You look at all the stuff we’ve done with laboratory animals, for example, and it’s pretty clear that helminths, if used in the right context, can be extremely beneficial.”
In the lab, helminth therapy has been shown to halt the progression of relapsing MS, relieve symptoms of IBS and celiac disease, and cure monkeys of chronic diarrhea. Speak to early adopters of the therapy and they’ll impress you with miracle stories of how it treated their previously untreatable illness, whether its allergies or ulcerative colitis. There are currently more than 4,000 people signed up to a Facebook support group.
However, not everybody is convinced. Yes, helminths have benefits over drugs currently prescribed to patients with autoimmune diseases, which are immunosuppressive and can put people at risk of developing cancer and other diseases. But they come with their own set of risk: The wrong worm in the wrong dose could trigger adverse side effects, including abdominal pain and weakness.
Take journalist Moises Velasquez-Manoff’s story as an example. Velasquez-Manoff took hookworms bought from Mexico to cure his alopecia and hay fever. At first, it seemed to work – his hay fever disappeared and patches of fuzzy hair began appearing on his body – but before long his hay fever returned and the hair stopped growing. The worms gave him cramps and diarrhea. These eventually cleared up but he was still feeling negative side effects months later.
Academically-speaking, the field received a major setback when a study examining porcine whipworms' effectiveness as a treatment for Crohn’s disease turned out to be a massive failure, with the helminths being no more effective than a placebo. No volunteers were harmed in the process and researchers now think they know what went wrong – the formulation was off. Still, the experiment’s failure combined with helminths’ ick factor and the million-dollar cost of tunneling a treatment through the FDA pipeline has delayed further research and scientists now struggle to access funding for future clinical trials.

Because there has been no large-scale double-blinded, placebo-controlled randomized trial, helminth therapy has not been approved by the FDA. Instead, intestinal worms are listed as an Investigational New Drug (IND), which basically means scientists conducting clinical trials are the only ones in the US allowed to distribute the treatment.
This has only forced people to move underground (or, rather, online). Suffering from incurable, frequently painful ailments, many patients with inflammation-caused medical problems are willing to give the therapy a go – with or without FDA approval.
Meanwhile, companies are setting up shop on the Internet to supply the increasing demand. One, called wormtherapy.com, was founded by a man called Garin Aglietti, who claims he cured his own psoriasis using hookworms acquired in Belize.

There is a big problem here: These businesses are largely unregulated. And while some people may be selling helminths because they genuinely believe in the health benefits, others who are more underhanded may be trying to make a fast buck without having to go through the usual oversight procedures. (After all, subscriptions can cost thousands of dollars.) Furthermore, people are self-administering treatments without medical supervision, which can be risky even among the well-informed.
What does Parker make of this? “To tell people you have to sit there and wait for the science while you have a disease that you know is going to kill you, that’s ridiculous,” he said. “We don’t condone doing it but at the same time we don’t say you should not go do this.”
“Obviously we would like them to be informed and be safe about it because there is a lot of information out there,” he added.
Given the current levels of interest (or rather, lack of interest) in helminth therapy from the established medical community, it looks unlikely we’ll see intestinal worms or pills made from their derivatives prescribed by your local doctor anytime soon. Yet, with increasing attention on helminths and other alternative treatments (such as fecal transplants) from people of the scientific community as well as members of the public, a worm-friendly future might not be as far off as you think.
In a few years, we might think of intestinal worms like we now think of bacteria – some are good, some are bad, and some are in-between. Though, as Parker admits, this shift in mindset could prove to be “a public relations challenge”.