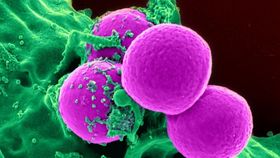
Staphylococcus aureus is an intimidating and challenging bacterium. It is responsible for a wide variety of human maladies, from annoying skin pimples to deadly meningitis. It’s pervasive and numerous strains have evolved antibiotic resistance, but perhaps most famously the “superbug” MRSA (methicillin-resistant S. aureus). While the arms race to fight them off continues, an international team of scientists has found a potential way to reduce the damage from infection. This could improve survival chances of patients with serious infections like pneumonia or the potentially fatal toxic shock syndrome.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.One of the most effective weapons in the bacterium's arsenal is the α-toxin, which pierces through the host cell membrane and can cause widespread tissue destruction. This research has identified the components of our cells that facilitate the havoc produced by the toxin. A significant culprit is the PLEKHA7 protein, which was discovered by the team of Sandra Citi, a professor at the University of Geneva (UNIGE) and co-director of the study.
To begin with, the team infected cells that did not have this protein with Staphylococcus aureus. Unlike normal cells, these were able to recover from the α-toxin-induced injury. They then moved on to animals that the researchers had genetically engineered to not express this protein, which told a similar story.
“Moreover, by infecting mice genetically deprived of PLEKHA7 with a multiresistant bacterial strain (MRSA), we observed improved healing from bacterial skin infection, as well as enhanced survival of pneumonia,” reveals Manuel Amieva, a professor at Stanford’s School of Medicine and co-senior author of the study, in a statement.
The team is trying to understand how PLEKHA7 is capable of affecting the virulence of the α-toxin. One of the hypotheses put forward in the study is that the protein transmits signals that promote cellular self-destruction, making the toxin, and thus the infection, significantly worse.
There are currently several approaches being studied to inhibit the PLEKHA7, and thus potentially limit Staphylococcus aureus. The discovery of an effective method could help reduce the damage of antibiotic-resistant strains of the bacterium.
The team, from Stanford University in collaboration with UNIGE, published its research in Proceedings of the National Academy of Science.