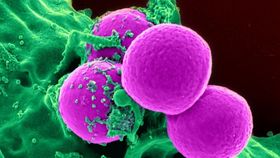
A technique borrowed from cancer treatment can perform a focused attack on microbes that are resistant to most antibiotics, according to new study published in Nature. Researchers attached an antibiotic to an antibody and found that the combination was highly efficient in fighting bacteria in mice.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.The team infected mice with methicillin-resistant Staphylococcus aureus (MRSA), which is one the most tenacious types of Staphylococcus (Staph). It then treated the mice either with the combination drug or with vancomycin, a powerful antibiotic that is often used against MRSA.
The researchers reported that the antibody-antibiotic conjugate (AAC) was about 1,000 times more effective against MRSA than vancomycin. It is believed that MRSA hides within cells, which often makes it difficult for antibiotics to defeat it.
“Most conventional antibiotics are fantastic at killing Staph outside cells, but poor at killing it inside the cell,” said Sanjeev Mariathasan from the biotechnology company Genentech in San Francisco, and a coauthor of the study, in a statement. “So the question was how do you kill the bacteria when it gets inside the cell?”
The AAC attaches itself to the bacteria as they're freely moving around the mice's bodies. Once the bacteria invade the cells, enzymes break the connection between the AAC components, enabling the antibiotic to kill the bacterium before it can do any damage.
Although a similar antibody-drug conjugation is being used to treat breast cancer, the AAC methodology might not be as effective in humans as it is in mice. The immune cells targeted by Staph are different in humans and mice. But if this method works in humans, it could lead to an entirely new approach in dealing with antibiotic-resistant bacteria.
Staph species are responsible for a large variety of conditions, from simple skin infections like pimples to deadly illnesses like meningitis. Every year, around 75,000 people are infected with MRSA in the U.S. alone, and around 10,000 of them die from it.