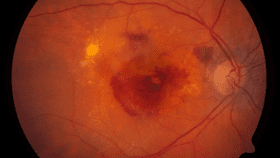
Hours ago, a Japanese woman in her 70s became the first human to receive a tissue transplant that was grown from induced pluripotent stem cells, RIKEN reported. The woman received a 1.3mm x 3mm sheet of retinal pigment epithelium as a treatment for her age-related macular degeneration, which diminishes the ability to register sharp, focused light.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Yasuo Kurimoto led the two-hour-long surgery at the Institute for Biomedical Research and Innovation in Kobe. Kurimoto reported that “there was no serious hemorrhaging or complication” involved with the surgery. Of course, it’s too early to tell how the transplant will take and how well she will recover, though previous research using animal models has not indicated that rejection or uncontrolled growth is likely to occur. Approval for using the technique was given just four days ago.
Pluripotent stem cells—often called embryonic stem cells—have the potential to become nearly any type of cell that the body may need. A number of chemical signals help determine what the cell may differentiate into down the line. Because of their wide potential, the cells are highly sought after to develop treatments for many diseases and conditions without the possibility for rejection that comes with transplanting donated tissues.
These stem cells are readily produced inside the blastocyst, which forms about five days after conception until implantation in the uterus. After implantation around day eight or nine, the inner cells will become the embryo, while the external cells become extra embryonic tissues, such as the placenta and amniotic sac. However, the source of the cells has been at the center of much controversy. Concerns about the sanctity of life and the ethical implications of obtaining these cells through IVF has led to high regulation and scrutiny.
Umbilical cord blood is packed full of multipotent stem cells, though they are not able to differentiate into quite as many different forms as pluripotent cells. Adults also have reserves of stem cells used for tissue regeneration, though their potential is limited to cell types found within a specific organ. Though these sources are more widely accepted, the narrow scope of possible cell types means they aren’t quite as good as the pluripotent cells from the blastocyst.
If scientists couldn’t obtain pluripotent cells from the source, they had to find a way to make them. In 2006, Shinya Yamanaka found a way to take normal adult body cells and subject them to four transcription factors that effectively turned back the hands of time and pushed them back into a state of pluripotency. Thus, induced pluripotent stem cells have all of the potential of embryonic stem cells, but with none of the contention.
Today’s surgery marks a dramatic step forward in the field of regenerative medicine and the role that induced pluripotent stem cells will play. Though the patient requested the utmost confidentiality and does not want to speak about her experience, it is hoped that this technique will be considered a great success, so that many others may be helped as well.
[Hat tip: David Cyranoski, Nature]
Read this: Scientists Create Solid Light
Correction: An earlier version of the article stated age-related macular degeneration can lead to blindness, which is not correct. Visual acuity can be drastically diminished with AMD, but does not cause complete blindness on its own.