Many of us are familiar with the grim experience of having the flu, from the clammy fever and body aches to the overpowering exhaustion. Usually, a couple of weeks is all we need to fully recover and feel symptom-free. An unlucky few, however, can experience reduced lung function for the rest of their lives due to changes to their lung tissue. Now, new research provides clues to what’s going on in their airways.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Bizarrely, researchers discovered that mice who’d experienced a severe bout of flu ended up with taste bud cells growing in their lungs. These cells are known as tuft cells or solitary chemosensory cells. They make up the taste buds and can be found in the throat and intestines too. But they’re not normally found in the lungs.
"It was just really weird to see, because these cells are not in the lung at baseline," said team leader Andrew E. Vaughan, a biologist at the University of Pennsylvania’s School of Veterinary Medicine. "The closest they are normally is in the trachea. What we did was show where they're coming from and how this same rare cell type that gives you all this maladaptive remodeling of the lung after flu is also the source of these ectopic tuft cells."
In previous research, Vaughan’s team uncovered cells responsible for the reshaping of lung tissue following the flu, describing them as lineage negative epithelial progenitors. The changes were accompanied by prolonged inflammation, a feature the researchers were keen to investigate. Their findings are published in the American Journal of Physiology.
In the new study, they looked at how mice’s lungs responded to a severe infection with the H1N1 strain of flu. The virus leads to a kind of immune reaction referred to as a Type 1 immune response. But strangely, a few weeks after the mice had recovered from their bouts of flu, their lungs showed signs of a Type 2 immune response. This kind of reaction is most commonly associated with allergies and asthma, as well as nasal polyps (small growths in the nose) and hookworm infections.
"These hallmarks of a Type 2 immune response after flu were unexpected, and have gone largely unnoticed until very recently," noted Vaughan.
So where do the seemingly misplaced tuft cells come in? Previous research has linked these cells to Type 2 immune reactions in the gut, so the researchers decided to see if they were also present in the lungs post-flu.
“And lo and behold, there they were, all over the place," said Vaughan.
“These recent findings may be a link between Type 2 inflammatory diseases, such as asthma, as well as nasal polyps, following a respiratory viral infection."
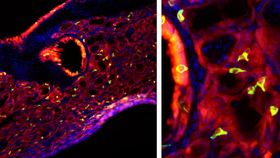
The researchers spotted the tuft cells in the lining of the airways and alveoli (tiny air sacs) of the lungs. They found that the lineage negative epithelial progenitor cells were precursors to the tuft cells.
When the team activated the tuft cells in the lungs of mice following a flu infection, they began to multiply, leading to acute inflammation.
While it’s important to remember that the new study is based on mice, not people, the researchers believe human lungs may be affected in the same way. Children who suffer numerous respiratory infections are more prone to asthma later in life, a condition linked to the presence of tuft cells.
While it’s still very early days, if these cells are found to be the culprits behind respiratory inflammation following severe flu in humans, future research could help us identify ways to prevent or treat it.