In a study published recently in Stem Cell Reports, a team of scientists have demonstrated that transplantation of human stem cells into disabled mice with a multiple sclerosis (MS) - like condition resulted in rapid and sustained clinical recovery. Within just two weeks of the treatment the mice were able to walk again, raising the possibility that this technique could eventually be applied to treat MS patients.
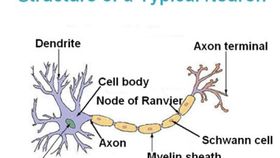
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.MS is a chronic and progressive inflammatory condition that results in the loss of myelin, the fatty insulating layer that forms around neurons. Myelin serves to ensure that electrical impulses that transmit information to and from the brain are transmitted efficiently. This demyelination and damage to neuronal cells results in a variety of clinical symptoms, from difficulty walking to blurred vision.
Over 2.3 million people worldwide suffer from MS, but current treatments have demonstrated little long-term benefit. There is therefore a need for therapies that bestow sustained improvements in patients, and previous studies using cell therapies in animal models have suggested that this could be a promising avenue.
In this current study, led by researchers at the University of Utah and The Scripps Research Institute in La Jolla, California, scientists imitated an MS-like condition in mice by inducing inflammatory-mediated demyelination in the central nervous system. They then transplanted human neural precursor cells (hNPCs) into the spines of the mice which were derived from human embryonic stem cells. Much to their surprise, within a mere two weeks of transplantation the mice started to exhibit dramatic clinical recovery.
“My postdoctoral fellow Dr. Lu Chen came to me and said, ‘The mice are walking.’ I didn’t believe her,” said co-senior author Tom Lane, professor of pathology at the University of Utah, in a news-release. The scientists witnessed a significant improvement in motor skill recovery of 73% of the mice, compared with only 14% in the control mice. Furthermore, the improvement in motor skills was sustained for 6 months after transplantation.
To gain a better understanding of the underlying mechanisms behind this recovery, the scientists investigated the spinal cords of the mice. They found that the mice exhibited a reduction in both inflammation and demyelination coupled with an increase in remyelination.
The scientists also predicted that the mice would reject the stem cells, and sure enough after 8 days they couldn’t detect any of the transplanted stem cells. This means that while the cells were indeed rejected they remained in the body long enough to exert an effect, which was likely through the release of certain chemical signals that stimulate repair or moderate inflammation.
“Rather than having to engraft stem cells into a patient, which can be challenging, we might be able to put those chemical signals into a drug that can be used to deliver the therapy more easily,” said Lane.
The team would therefore like to continue their work by identifying these factors that are released by these cells with the ultimate goal of developing an MS therapy, ideally cell-free, which can be put forward for clinical trials.