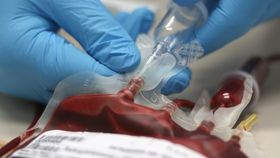
During the 70s and 80s, thousands of people around the world were infected with HIV and hepatitis C after receiving transfusions of blood containing these viruses. Back then, screening wasn’t so stringent, nor was the assessment of who is eligible to donate. Now we have better techniques to identify such agents, we should be able to avoid catastrophes like these from happening, which is why a team of scientists has been on the hunt for new transfusion-transmissible agents that we might want to know about.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.And they managed to find one: the previously unknown human hepegivirus 1 (HHpgV-1), as it has been named. Although the study, published in mBio, demonstrates the potential of this virus to be passed on by blood products, we needn’t get our knickers in a twist just yet. It was only found in a small number of people, some of whom managed to get rid of it, and it has yet to be associated with disease.
The discovery was made after a team of scientists from Columbia University used highly sensitive sequencing techniques to look for changes in the viromes – the viral equivalent of the microbiome – of people given blood transfusions. Samples, both pre- and post-transfusion, came from a total of 44 individuals, all of whom had enrolled into a study on transfusion-transmitted viruses between 1974 and 1980.
After plowing through millions of reads (the viral sequences detected), they came across two individuals who appeared to be infected with a novel virus, but it was only found in their post-transfusion samples. Further analysis revealed that the virus belonged to the same family as hepatitis C virus (HCV) and another virus called human pegivirus – the flaviviruses. While the former can cause deadly liver disease and cancer, the latter, which was previously called hepatitis G virus, actually seems to help HIV patients live longer. Not only do three of its proteins seem to block HIV replication, but the immune systems of individuals co-infected with these viruses seems to be reined in, avoiding excessive activation that actually helps HIV flourish.
In both of these patients, samples taken the day before transfusion and around eight months later were negative for HHpgV-1, which not only suggests that the virus could be transmissible by transfusion, but also that the patients managed to clear it. Neither of these individuals seemed to present any kind of associated disease either.
The researchers then looked at another group of 106 individuals who had received blood transfusions for the bleeding disorder hemophilia. Two of these patients tested positive for HHpgV-1, but this time both of them had persistent infections, one lasting a minimum of 201 days, the other 5.4 years. Again, there were no obvious illnesses linked with infection.
Although we know a lot of about the family of viruses to which belongs, we must be careful about drawing inferences when HHpgV-1 hasn’t even been isolated or grown in tissue culture yet, nor do we know how prevalent it is in the general population. Furthermore, just because it’s a human virus, that doesn’t mean we should immediately fear it. Our bodies are absolutely riddled with viruses, just like they are with bacteria, so it’s likely we will find many more as sequencing techniques improve. Still, further studies are warranted to investigate its potential to cause disease, which may lead to even tighter blood screening processes.