Nanoparticles are a highly desirable approach to treating cancer, as it can target the diseased cells while leaving the healthy cells alone. This is quite an improvement on traditional systemic chemotherapy treatments. New nanoparticles can even hold multiple drugs at once, increasing the efficacy of the treatment. Now, a team led by Paula Hammond and Michael Yaffe at MIT have developed nanoparticles that can time the delivery of the second drug to when it would be most effective. The results were published in Science Signaling.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Many cancer patients receive multiple drugs at the same time when fighting the disease, in order to receive the best chance at recovering and it was relatively recently that Yaffe’s lab discovered that the timing of when these drugs are administered can drastically improve their efficacy. The first drug primes the cell by shutting down certain metabolic pathways, which allowed the second drug to come in and damage the tumor cells’ DNA more effectively than if both drugs were administered together. This knowledge of timing when combined with the precision of nanoparticles could be an incredibly improved method of treating cancer, while minimizing harmful side effects.
“I think it’s a harbinger of what nanomedicine can do for us in the future,” Hammond said in a press release. “We’re moving from the simplest model of the nanoparticle — just getting the drug in there and targeting it — to having smart nanoparticles that deliver drug combinations in the way that you need to really attack the tumor.”
The first drug administered is erlotinib, which targets the epidermal growth factor receptor, prohibiting the growth and replication of the cell. It is currently approved for treatment in pancreatic and some lung cancers. The second drug, doxorubicin, works on the intercalation of the tumor DNA, prohibiting protein synthesis, and is currently used to fight a wide variety of cancers.
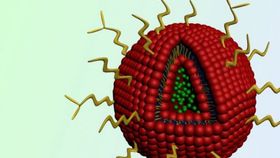
The team found that the most effective design to transport the drugs were liposomes: hollow spheres with a lipid bilayer husk. The erlotinib was put into the liposome’s outer layer, with the doxorubicin held inside. Each unit was coated in PEG to stop the body from breaking it down prematurely. As tumor cells have abnormally high folate receptors, folate was used to help guide each nanoparticle toward the diseased cells. When the nanoparticle binds to the tumor cell, it starts to break down. The erlotinib is administered first and prepares the cell for the doxorubicin, which will be most effective about 4-24 hours later.
This drug delivery system was given to mice who had implanted tumors from human breast and lung cancer which are very aggressive. The tumors became significantly smaller following treatment, even when compared to mice who had the drugs administered together. Before this approach can be taken to human trials, it will need to be tested on mice who develop cancer naturally, and are not just acting as a host for human cancers.