It’s clear that obesity can have a damaging effect on your heart, lungs, liver, and many other precious bodily organs, but what about your brain?
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.New research has found that the brains of obese teenagers appear to show signs of damage. These visible changes to the brain could also change people’s cognitive and emotional functions, which could, in turn, reinforce cycles of behavior associated with overeating and obesity.
Speaking at the Annual Meeting of the Radiological Society of North America next week, the researchers from the University of São Paulo in Brazil will present their study investigating the difference between the brains of obese and healthy teenagers.
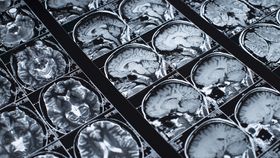
The team carried out MRI scans on the brains of 59 obese adolescents and 61 healthy adolescents. They specifically used a technique known as tensor imaging (DTI) to analyze the condition of the brain's white matter, the tissue containing the connecting branches of neurons, sometimes thought of as the "superhighway" between brain regions.
The findings, which haven't yet been published in a peer-reviewed journal, showed that obese adolescents tended to have damage in the corpus callosum, a bundle of nerve fibers that connects the left and right hemispheres of the brain. The quality of the white matter was also lower in the obese teens’ middle orbitofrontal gyrus, a brain region related to emotional control and the reward circuit – an intriguing find given the link between obesity and abnormalities in the brain’s reward circuit.
"Brain changes found in obese adolescents related to important regions responsible for control of appetite, emotions and cognitive functions," study co-author Pamela Bertolazzi, a biomedical scientist and PhD student from the University of São Paulo in Brazil, said in a statement.
The cause of the damage, according to the researchers, appears to be inflammation. They found that the levels of damage tended to correlate with marks of inflammation, such as leptin, a hormone made by fat cells linked to energy levels and fat stores. Some obese people also develop leptin resistance, which can prompt them to eat despite having abundant fat stores. This can make losing weight a struggle.
Poor white matter quality was also related to heightened levels of insulin, a hormone released in the pancreas to control glucose (sugar) levels in our bodies. Equally, some obese people often suffer from insulin resistance, leading to issues with blood sugar regulation.
"Our maps showed a positive correlation between brain changes and hormones such as leptin and insulin," Dr Bertolazzi said. "Furthermore, we found a positive association with inflammatory markers, which leads us to believe in a process of neuroinflammation besides insulin and leptin resistance."
This is not the first study to highlight the link between obesity and brain health. A 2016 study looked at the brains of overweight middle-aged people and found their white matter appears 10 years older than those of slim people of the same age. These profound changes were also visible in their brain scans.