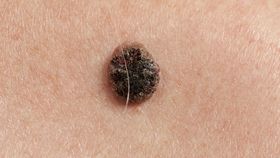
A doctor has injected a woman whose skin cancers were too widespread to be treated in other ways with Gardasil. Not only did the cancers clear up, but they have not reoccurred since. Although case notes from a single patient are no match for controlled trials, the outcome raises the possibility the much-derided vaccine could be saving even more lives than we realized.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Squamous cell carcinoma is the second-most common type of skin cancer after basal cell carcinoma. While not as deadly as melanoma, it still accounts for thousands of deaths each year worldwide, along with much suffering.
Certain strains of the human papillomavirus (HPV) are known to cause almost all cervical cancers, as well as many cancers of the anus, vagina, and vulvar. The presence of the virus in many squamous cancer cells alerted medical researchers to the likelihood that some skin cancers could be added to this list.
In 2017, Dr Anna Nicols of the University of Miami reported that, after being given the anti-HPV vaccine Gardasil, two people who suffered from squamous cell cancers experienced fewer new cancers. Inspired by this success, Nicols' colleague Dr Tim Ioannides suggested injecting Gardasil directly into skin tumors to see if it could also kill existing cancers.
Most squamous cell cancers are treated through surgery, radiation therapy, or both. However, one of Nichols' patients was a 97-year-old woman whose leg had so many tumors none of these options were considered safe. Nichols got approval from the patient to inject two doses of Gardasil in her arm, six weeks apart, followed by injections into several of the tumors, repeated over a period of 11 months.
"I think we had a really reasonable expectation and good data that this was actually going to, at the very least, do no harm to this patient, and possibly provide some benefit," said Ioannides in a statement.
They got something much better. "All of her tumors completely resolved 11 months after the first direct tumor injection, and she has had no recurrence," Nichols said. "It has been about 24 months now since we started with the treatment." The patient, who will soon turn 100, is understandably delighted.
The work, reported in JAMA Dermatology, raises the possibility that Gardasil could be used much more widely in treatment, being much less invasive than existing options. Moreover, it seems possible the widespread provision of Gardasil to prevent cervical cancer could be causing an as-yet unmeasured reduction in skin cancers.
The campaign against Gardasil has been even more virulent than against other vaccines, combining extraordinary exaggeration of side effects with denial of its success against cervical cancer. It's possible these falsehoods are doing even more damage than anyone realized.