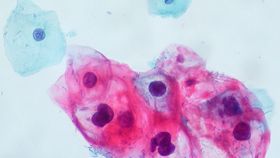
A controversial mass vaccination campaign against the human papillomavirus (HPV) has paid off, making sex safer even for unvaccinated young people with benefits that could last for 70 years. The findings could teach us a lot about how to deploy vaccines against other diseases.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.The most damaging of HPV's many strains cause genital warts and trigger changes to cells in the cervix, anus, and even throat that can eventually become cancerous. The announcement of a vaccine brought hope for preventing hundreds of thousands of deaths each year.
Anti-vaxxers and those who hope sexually transmitted infections will discourage sexual activity were opposed of course. However, even many epidemiologists questioned whether the widespread use of such an expensive vaccine was good value for money.
Governments worldwide responded differently as to how widely to promote the vaccine, creating a natural experiment that has allowed scientists to learn lessons for future vaccines.
The vaccine was based on Australian research, and possibly as a reflection of national pride, Australia was the most enthusiastic adopter, providing a test case for everyone else. A study in the Journal of Infectious Diseases suggests they got it right. Most countries either vaccinated erratically, or concentrated on girls aged 12-13, who were very unlikely to have been exposed to the virus. Australia offered free catch-up vaccinations for women under 26 leading to 1.5 million vaccinations in three years.
Cervical cancer takes a long time to manifest, which has delayed assessing the campaign's success. “We are entering time frame when we expect to start seeing impact on cancer,” Dr Julia Brotherton of the Victorian Cytology Service Registries told IFLScience.
However, HPV-induced cancers are so rare for women in their 20s the Australian sample is probably too small to measure the fall. Genital warts appear more quickly, and previous research has shown a spectacular fall in their occurrence as a result of the vaccination campaign.
Brotherton found the 90 percent decrease in genital warts among women aged under 21. Australia has seen that would have been just 38 percent without the catch-up program. A decline in other HPV-induced cancers such as the head and neck cancers transmitted through oral sex, will take even longer than cervical cancer to be seen, Brotherton told IFLscience.
According to Brotherton, part of the drop is because even people who were not vaccinated are benefiting from herd resistance, as their sexual partners are unlikely to carry the virus if they, or their previous partners, were vaccinated.
The herd resistance, at least for predominantly heterosexual populations, operates very differently from diseases where anyone can spread to anyone. However, Brotherton says the way vaccinated women formed a barrier preventing their male partners from becoming infected could serve as a great model for heard resistance for future vaccinations against STIs.