In their most primitive state, stem cells have the ability to become almost any cell in the body – muscle, blood, bone, nerve, and so on. The use of these cells has the potential to revolutionize medical treatments, from regenerating damaged heart tissue after an attack to creating insulin-generating cells for a malfunctioning pancreas.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Now, a team of researchers from the University of Cambridge has shown for the first time that one of the most flexible types of stem cell can be derived from human embryos. These so-called naïve cells can turn into any other type of human tissue with the sole exception of the placenta. The groundbreaking study, published in Stem Cell Reports, reveals that this new technique could open up brand new avenues in medical research, and potentially boost our understanding of disorders like Down’s syndrome.
The most sought-after stem cell type tends to be the human “pluripotent” variant, which is able to become (or “differentiate” into) a wide range of specialized cell types at the whim of a researcher. They’re derived from two sources: embryonic stem cells, which come from fertilized eggs discarded from in vitro fertilization (IVF) operations, and skin cells that are reprogrammed to become pluripotent stem cells.
These cells have already been “primed” to differentiate into specific cell types, however. The most basic form of pluripotent stem cell aren’t primed at all, and these “naïve” cells can be easily programmed to become any cell type. Although these naïve cells can be derived from mouse embryos, it was unknown until now if they could be developed from human embryos.
As this new study reveals, researchers have been able to steal away these naïve cells from a human embryo on the sixth day of its natural development. By this point, a structure called a blastocyst has appeared, which will normally go on to form the placenta, the “yolk sac” that provides nutrients to the developing fetus, and the naïve cells that will ultimately form the future body.

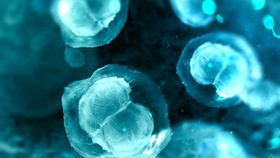
Colonies of human naïve embryonic stem cells produced using the new technique. Ge Guo
The team employed a technique known as “immunosurgery,” which carefully removes specifically-designated external cell layers of objects – in this case, the object was the blastocyst. By removing its outer layer, the naïve cells were exposed and able to be extracted. They were then grown individually in the laboratory; this forced separation prevented them from communicating with each other, which stopped them automatically differentiating into specialized cell types.
Although mouse-derived naïve stem cells have displayed remarkable abilities when injected back into mice, human-derived naïve stem cells could lead to genuinely game-changing medical treatments for people. Organs like the heart, brain, and pancreas have incredibly poor regenerative capabilities, and as a result are unable to recover from serious damage. In theory, these new, easily programmable naïve cells could be used to restore their long-lost regenerative abilities.
Additionally, these naïve cells could be intentionally cultured to differentiate into an “affected” line of cells, one that would lead to debilitating conditions like Down’s syndrome. This disorder appears when an extra copy of chromosome 21 is erroneously made, which takes place during the development of a fertilized egg. By comparing a “healthy” and “affected” cell line grown from naïve cells, new insights into the origin of Down’s syndrome could be made.