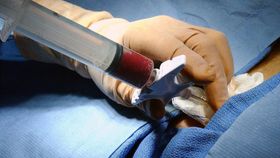
Currently, patients receiving treatment for leukemia are given six months of immunosuppressant drugs. However, a study at Johns Hopkins Kimmel Cancer Center indicates that complete suppression of the immune system after a bone marrow transplant can be avoided. Patients can be given two days of cyclophosphamide, allowing their immune systems to return to their job of protecting against other diseases.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Bone marrow recipients are at risk of grave-versus-host-disease (GVHD), where the body's immune system attacks the transplant, treating it as if it were an infection. Normally this is countered by weakening the immune system, which involves a lot of risks.
In the Journal of Clinical Oncology, a team led by Dr. Leo Luznik followed 92 patients with high-risk blood cancers. All received bone marrow transplants from matched donors. In 45 cases, the donors were close relatives while the rest came from bone marrow registries.
Instead of using the usual immunosuppressent drug regimes, those in the trial were administered two chemotherapeutic drugs, busulafan and fludarabine, before the transplant and two days of cyclophosphamide afterwards.
Almost half of the bone marrow transplant recipients on the conventional regimes developed chronic GVHD, some of whom died as a result. In this trial however, only 14% developed chronic GVHD, while 15% suffered severe acute GVHD and another 36% experienced the milder (grade II) form of the acute condition. In some cases, however, it was necessary to supplement the cyclophosphamide with other immunosuppressant drugs. Rates of GVHD were no different for those receiving donations from relatives or unrelated donors.
Luznik noted that the acute responses were similar to those using mainstream treatments, while the chronic cases of GVHD were much rarer with the cyclophosphamide, in addition to the benefit of patients having their immune systems restored more rapidly. The latter, he said, "also allows for the earlier integration of other treatments."
"If you give patients immune cells to eradicate any remaining cancer cells that might be present, those immune cells would not be prevented from doing their job by ongoing immune suppression drugs that are being used in patients treated with conventional transplant approaches," said first author Dr. Christopher Kanakry.
Oncologist Dr. Koen van Besien of Weill Cornell Medical College, who was not involved in the study, said in a Journal of Clinical Oncology podcast,“Many modifications have been studied in an attempt to improve outcomes,” for established methods for preventing GVHD, but “none of these have been superior.”
Two years after the operations, the team found that 67% of the patients were still alive and 62% cancer-free.
As a result of earlier work by Luznik, cyclophosphamide is now often given when no fully matched donor marrow can be found, but this has been done in conjunction with other drugs, rather than instead of them.
Van Besien explains that the Luznik's trial worked because, as Luznick previously showed, “Cyclophosphamide when given in high doses eliminates proliferating alloreactive t-cells but spares regulatory t-cells.”
The team is planning phase III randomized trials.