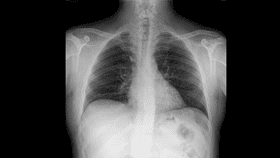
Despite reaching nearly every corner of the world, there is much to be known about SARS-CoV-2, including a fully representative characterization of how the respiratory disease manifests within the lungs.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.To enhance scientific understanding of the varying impacts of coronaviruses on the lungs, researchers reviewed pediatric lung disorders, including those that occurred as a result of coronaviruses like severe acute respiratory syndrome (SARS), Middle East respiratory syndrome (MERS), and those associated with Covid-19.
“The early 21st century has seen the emergence of several severe outbreaks of pediatric lung illnesses such as contagious viral epidemics, including three coronaviruses,” wrote the authors in the American Journal of Roentgenology. “Because of their immature lung anatomy and developing immune systems, pediatric patients are often particularly susceptible to these public health crises.”
Diagnosing child lung disorders can be challenging due to the vague, overlapping symptoms and the difficulty or inability of young children and infants to describe their symptoms. Children diagnosed with SARS tend to have milder presentations of the disease than adults, with more than one-third of children found to have “normal findings” on their chest radiographs. In those that did show symptoms on scans, the lungs were patchy ground-glass opacities, small obscurities that indicate obstructions in the lung. A normal CT scan should appear black, but obstructions in the organs are depicted as white blockages.

An 8-year-old boy with SARs who went to the hospital after experiencing fever and chills. A frontal CT scan shows a small space of opacification (left) and an increase in opacification two days later (center). An axial view taken seven days after being admitted to the hospital shows airspace consolidation and ground-glass opacity. American Journal of Roentgenology
Those diagnosed with MERS similarly saw reports of ground glass opacity. In extreme and often fatal cases, children saw pneumothorax, or a collapse of the lung, and pleural effusion – “water on the lungs” indicating an excess buildup of fluid. Both symptoms can serve as an important indication of diagnosing fatal cases.

The frontal chest radiograph of a 12-year-old diagnosed with MERS shows ground-glass opacities, as well as a tracheostomy tube to assist with breathing (left). A 20-year-old showed similar ground-glass opacities. American Journal of Roentgenology
As with SARS and MERS, CT scans of patients exhibiting symptoms of Covid-19 can help doctors diagnose the disease and determine its impact on the body, particularly as testing kits are largely limited across parts of the world and the accuracy of those that are available are known to produce a high rate of false-negative results, leading to delayed treatment.
“Chest CT has been shown to have a significantly higher rate of sensitivity in detection of SARS-CoV-2 than the initial reverse transcription-polymerase chain reaction test,” write the authors. “In fact, during the outbreak in China, chest CT findings were added as major evidence for confirmed clinical diagnosis.”

CT scans of a 16-year-old girl diagnosed with Covid-19 with a known history of tuberous sclerosis shows initial consolidations and ground-glass opacities (left) as well as increased consolidations in the lower lung zones (center). A frontal CT shows some improvements six days after hospital admittance. American Journal of Roentgenology
Although a chest radiography is typically the first imaging study in patients believed to have Covid-19, the researchers note that there is not a lot of published information describing the appearance of these scans. Across the studies analyzed, chest CTs showed lung parenchymal abnormalities, consolidative opacities, ground-glass opacities, and unilateral patchy opacities. Patients diagnosed with both pneumonia and Covid-19 were also more likely to experience vascular thickening and a “reversed halo” sign than those with pneumonia alone. In children, the most frequently observed abnormalities were subpleural lesions, unilateral or bilateral pulmonary lesions, ground-glass opacity, and a consolidation that resembles a halo sign.
“A clear understanding of the imaging manifestations of these pediatric lung disorders is essential so that the radiologist can make a timely and accurate diagnosis,” conclude the researchers.
Although there are some overlapping imaging features of the various lung disorders analyzed, careful evaluation of their unique presentations can “allow the radiologist to offer a narrower differential diagnosis in pediatric patients, leading to optimal patient care.”

Additional CT views show the ground-glass opacity and consolidation (left) and “small component of consolidation” (right) in the lower left lobe of the lung of a 16-year-old girl. American Journal of Roentgenology