A 25-year-old woman was rushed to the emergency room after she fell sick and her skin turned a faint blue hue. To the surprise of doctors, it emerged that her blood had also turned a dark shade of navy blue.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.A case study published in the New England Journal of Medicine documents the unusual case that emerged at Miriam Hospital in Rhode Island. Doctors working on the case explain that the bizarre coloring was the result of medicine used to treat toothache.
Shortly before going to bed the previous night, the woman had used a “large amount” of topical pain reliever for a toothache that contained benzocaine, a local anesthetic, or numbing medication. She woke up feeling weak, tired, short of breath, and with skin discoloration, so wisely took herself to the hospital.
Doctors noted that she had a respiratory rate of 22 breaths per minute (a relatively normal level ) and a dramatically low oxygen saturation of 88 percent. For context, you should expect a normal healthy oxygen saturation level to be between 97 and 100 percent. She was given supplemental oxygen, but this failed to resolve the problem and her oxygen saturation slipped to 67 percent.

She was eventually diagnosed with acquired methemoglobinemia, a condition in which an abnormal amount of methemoglobin is produced. Methemoglobin is created when the iron in a person’s hemoglobin, the protein in red blood cells that carries and distributes oxygen to the body, changes form. The altered protein cannot bind oxygen, which means it cannot carry oxygen to tissues.
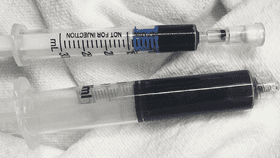
Contrary to popular belief, deoxygenated blood is not bright blue like the color of your veins. It is true that oxygenated blood is a brighter red color due to the presence of oxygen-loaded hemoglobin. When hemoglobin releases oxygen, its shape changes and the protein appears darker, causing deoxygenated blood to turn dark red. In this case, the blood was so deoxygenated it appears extremely dark, almost black with a very mild tinge of navy blue.
While it’s not completely clear why the painkilling drug caused the woman to develop methemoglobinemia, the reaction is not unheard of. The US Food and Drug Administration (FDA) notes on its website that "consumers using benzocaine products to treat mouth pain should seek medical attention immediately for signs and symptoms of methemoglobinemia.” Around 319 people have been treated for benzocaine-related methemoglobinemia in the US. Three people have died.
Fortunately, the woman made a recovery from her perilous day in the ER. She was treated with intravenous methylene blue, the go-to treatment for methemoglobinemia, and promptly experienced a considerable improvement in her breathing, as well as a reduction in skin discoloration.