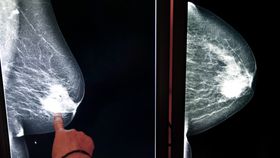
Two cheap generic drugs could cut breast cancer deaths in postmenopausal women with early stages of the disease. Researchers suggest that two classes of drugs – bisphosphonates and aromatase inhibitors (AIs) – could be used together to complement one another, increasing the benefits and reducing some of the side effects.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.About two-thirds of all women who go on to develop breast cancer are postmenopausal and around 80% are hormone sensitive. While surgery can remove detectable cancer from the breast, there’s still a risk some undetected micro-tumors that are too small to see can be left behind. The drugs detailed in two studies published in The Lancet medical journal have the potential to reduce breast cancer deaths, researchers say.
In the first study, researchers investigated the effect of treating postmenopausal women with a newer endocrine therapy – an AI. The study was a meta-analysis, looking at previous data from nearly 32,000 postmenopausal women in nine randomized trials. Researchers found that compared to tamoxifen, a common drug to treat breast cancer, AIs were able to reduce the likelihood of the cancer recurring by about a third over a five year period. AIs also reduced the risk of dying by around 15% over the course of a decade. When AIs were compared to no treatment at all, the reduced risk of dying shot up to 40%.
There are, however, some side effects to taking AIs. Dr. Aine McCarthy, Science Information Officer at Cancer Research UK, tells IFLScience that AIs can cause a reduction in bone density. This is why researchers are suggesting that two types of drug be used together, as the side effects on bone health can be alleviated by taking bisphosphonates – a relatively cheap drug normally used to prevent bone loss in osteoporosis.
In the second study, researchers demonstrated that bisphosphonates could reduce secondary tumors growing in the bone by 17% in the overall study population. That effect was even greater in postmenopausal women, as researchers found that two to five years with bisphosphonates reduced recurrence of cancer in the bone by 28% and cut death rates by 18% over the 10 years.
“What can happen at the moment is that if a woman’s cancer spreads to her bones she can be given bisphosphonates if she has a low bone density. What this study is suggesting is that women should be given bisphosphonates up front from the start,” McCarthy explains.
“These results are very encouraging because 18% decrease in mortality roughly equates to saving a 1,000 lives a year and that’s a huge.”
Researchers stress that the positive results were seen in postmenopausal women, and the same effects were not seen in younger women who had yet to go through menopause. The study was a meta-analysis of 26 separate trials, which included individual patient data on nearly 19,000 women.
“These are encouraging results and based on this evidence we’re recommending that NICE [The National Institute for Health and Care Excellence] needs to look at this and see whether these two drugs should be given as treatment to post-menopausal women with early breast cancer,” McCarthy says.
McCarthy says that further research is still important “to better tell us to how to give these drugs in combination with each other.”