In medicine, there is often the concern that a patient will not respond to a particular treatment, but in a turn for the books, physicians are now worried that a new cancer treatment might be so effective at eliminating tumors that it does more harm than good.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.After receiving a single treatment of a novel combination therapy, a woman’s tumor seemingly “dissolved” from her chest in just three weeks, leaving her with a gaping hole in its place. The patient received the same cocktail of skin cancer drugs as almost 150 individuals enrolled in a clinical trial designed to test whether one of the therapies worked better on its own or when combined with another. While most patients did significantly better on the combination therapy, researchers were left gobsmacked by this woman’s rapid and dramatic response and have consequently described her case in the New England Journal of Medicine, alongside the trial results.
The therapies the scientists were investigating were the FDA-approved melanoma drugs Yervoy (ipilimumab) and Opdivo (nivolumab), which are both antibodies. The former works by interfering with a molecule that can switch off a type of cancer-fighting immune cell called a T-cell, whereas the latter blocks a pathway that can lead to the death of T-cells. Although they act in different ways, both drugs ultimately stimulate the immune system to fight cancer cells.
For the trial, 142 patients with melanoma that had spread to other parts of the body, or metastasized, were randomly assigned either Yervoy plus a placebo or Yervoy in combination with Opdivo. They found that, overall, patients in the combination group fared significantly better than those receiving Yervoy and the placebo. Fifty-three percent of these patients experienced at least 80% tumor shrinkage, and melanoma became undetectable in 22% by the end of the study—a remarkable response for stage IV cancer. None of the patients in the Yervoy monotherapy group achieved this outcome.
Although the trial is now over, it has been extended so that some advanced melanoma patients can still access the combination treatment, which is how the woman described earlier managed to receive the treatment, Live Science reports. According to the case report, the 49-year-old had undergone both surgery and chemotherapy to treat melanoma over a period of four years. Although she had several tumors removed, the disease was persistent and five months ago she developed a large mass under her left breast, which was presumed to have spread from the primary melanoma on her back.
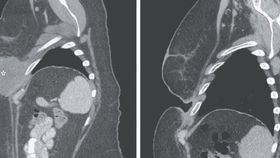
She was given a single dose of the new combination therapy, but when she returned for her second just three weeks later, she reported that her tumor had “disappeared.” Alongside the obvious hole in her chest, CT scans confirmed that the large tumor had been completely eradicated. While such a rapid and dramatic response may sound desirable, the researchers have expressed concerns since if this were to happen to a tumor elsewhere in the body, such as the bowel or heart, it could have grave consequences.
“It is ironic that we are now concerned about the possibility of overly vigorous antimelanoma responses,” the researchers write.
[Via NEJM and Live Science]