We've heard of light relief, but this is new. A novel technology demonstrated in mice could cause the nerve cells of the intestinal walls to respond to illumination. By placing tiny LEDs inside the gut, muscles could be made to work, ending constipation without the many side-effects of current treatments. The idea of having light sources rectally inserted, and your neurons modified to respond, may seem drastic, but those suffering from chronic constipation – an increasing problem with age – may consider it worth it.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.“A 65-year-old human has about half the neurons in their intestines as a person of 35,” Professor Nick Spencer of Flinders University in Australia told IFLScience. The loss of neurons is just one reason why the muscles that surround the intestine can fail to work, leaving people with the unpleasant symptoms of chronic constipation. When exercise and diet fail, drug treatments can have side-effects almost as bad as the condition itself.
Spencer is hoping the emerging field of optogenetics can provide an answer. Channelrhodopsins are light-stimulated ion channels borrowed from algae that induce responses in cells when exposed to particular wavelengths of light. These channels have been introduced into animals for study purposes through genetic modification, but Spencer told IFLScience other methods are available for humans.
“The technology uses a harmless virus that has already been approved for cancer therapy,” Spencer said. “It acts as a vehicle to transport light-sensitive ions along the nerve axons.” A month or so later, Spencer said, LEDs would be implanted to stimulate the relevant neurons, causing them to fire at the appropriate times and the muscles to contract.
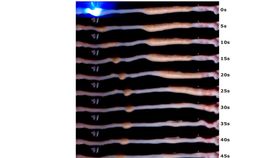
Spencer described the success of this idea on mice in Gastroenterology, using implanted blue LEDs to induce movement of stools through the intestine, leading to a 75 percent increase in fecal droppings over the subsequent 15 minutes, compared to a control group.
The work focused on the gut because, Spencer said, it is the only internal organ besides the brain and spinal cord with an independent nervous system.
An even more ambitious plan is to extend the idea to other internal organs experiencing chronic pain. For these, the light would be used to inhibit, rather than stimulate, the neurons, so that a sufferer could dial down their sensitivity in only the relevant organ rather than relying on painkillers that affect the entire body, usually in undesirable ways.
Spencer added that, while the process of sensitizing neurons to light may not be permanent, there have been studies showing the effects remain after 18 months. Since no testing has been done over longer time frames we don't know when degradation takes place, if at all, but it is unlikely treatment will need to be frequent.
The insertion of light sources into the body sounds painful, but Spencer says it is no more radical than the use of heart pacemakers. The lights themselves and an induction coil all fit on a chip less than 2 millimeters (0.08 inches) wide. Microwaves, similar in frequency to those used by mobile phones rather than the ones in an oven, could be supplied from an outside power source to generate current in the induction coil. The user could flick a switch on a wearable powerpack to turn on their internal lights, stimulating the targeted cells to make their muscles work or pain subside.