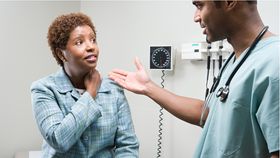
Placebo is a powerful phenomenon wherein the power of suggestion gives fake or ineffective treatments healing properties. Because the effect hinges entirely on one’s beliefs, pretty much anything from sugar pills to juice cleanses to GOOP products can make people feel better.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.And given that we tend to trust the expertise of physicians and other healthcare providers, it’s not too surprising to hear that past studies have found medical professionals can influence their patients’ responses to both real and bogus medicines by offering encouragement and a positive prognosis.
Now, thanks to a new study from Stanford University, there is evidence that words alone may do the trick.
In an ingeniously simple experiment, lead researcher Alia Crum and her colleagues showed that people who were told that their allergic reaction would soon subside reported an immediate reduction in symptoms.
“Physician assurance is a component of medical care that is surely familiar to physicians, yet is under-researched and often under-appreciated,” they wrote in the Journal of General Internal Medicine.
“Although meeting with patients for issues not ultimately requiring medication or treatment may be seen as costly or unnecessary from a health economics perspective, this study highlights the critical yet rarely quantified healing effect of visits in which the physician’s sole role is to assure patients they will soon feel better.”
The study involved 76 participants who were taken into a room one by one and administered a histamine skin prick – a harmless procedure that induces temporary itchiness, swelling, and redness – on the forearm. After three minutes, the healthcare provider who had given the jab came back and asked the participant to rate how itchy they felt on a scale of zero to 100.
Then, the provider visually examined each participant's arm, and to those who had been randomly assigned to the “assurance” group, the provider said: “From this point forward your allergic reaction will start to diminish, and your rash and irritation will go away”. No comments were made to participants assigned to the control group. The provider returned and asked for itchiness ratings again at the nine, 12, 15, and 18-minute marks, but made no additional comments to subjects in either group.
Looking at the scores, Crum’s team saw that the assurance participants reported significantly lower scores than the control participants (20.2 vs 29) just six minutes after the positive words were shared. Overall, a difference in average rating persisted between the two groups, but the magnitude decreased as time went on; an expected outcome seeing as histamine jabs itch less and less as the reaction dissipates.
Although the study presents preliminary findings that will need to be substantiated with larger studies before recommendations for clinical care can be established, Crum believes it is an area worth pursuing.
“Going to the doctor is largely a psychological experience,” Crum said in a statement. “Often we simply want to be reassured that what we are experiencing is ‘normal’ and will go away. And yet, the response we often get is complicated diagnoses, expensive medications and added uncertainty, all of which may not only fail to harness psychological aspects in healing but may actually generate mindsets that could make us feel worse.
“My hope is that findings like this one inspire additional research on the physiological mechanisms of assurance as well as promote training and compensation for physicians to more effectively leverage psychological forces in their practice.”