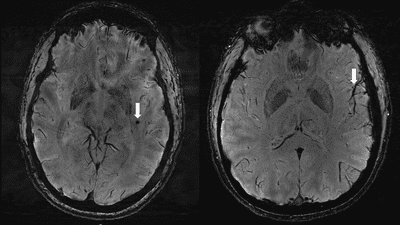
Unique brain changes seen only in people who get migraines have been discovered and could open up new avenues for further research into the management of the often debilitating condition. For the first time, researchers have confirmed changes that sit within an area of the brain called the centrum semiovale, the central area of white matter that sits underneath the cerebral cortex.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Our brains contain perivascular spaces, fluid-filled gaps that surround blood vessels and are found in several organs. In the brain, they’re crucial for the organ’s fluid clearance system – called the glymphatic system – and so finding out if and how they are linked to migraine could help doctors to better understand why some people get them.
The study scanned 10 people with chronic migraine, 10 with episodic migraine without aura, and five controls who didn’t experience migraine to look for differences. As well as checking for changes in the perivascular spaces, they were looking for white matter hyperintensities: a type of lesion that’s seen in people who get migraines.
Scans revealed that there were significant changes in the perivascular spaces within the centrum semiovale in the participants who got migraine. For this group, the quantity of these changes was correlated to the presence of white matter lesions.

“We studied chronic migraine and episodic migraine without aura and found that, for both types of migraine, perivascular spaces were bigger in the centrum semiovale,” said study co-author Wilson Xu, an M.D. candidate at Keck School of Medicine of the University of Southern California in Los Angeles, in a statement.
“Although we didn’t find any significant changes in the severity of white matter lesions in patients with and without migraine, these white matter lesions were significantly linked to the presence of enlarged perivascular spaces. This suggests that changes in perivascular spaces could lead to future development of more white matter lesions.”
“These changes have never been reported before.”

Given the physiological role of perivascular spaces, it’s possible that significant changes to its structure could disrupt the glymphatic system. This would effectively mean the brain is unable to wash itself properly, leading to a build-up of waste metabolites that can be toxic to the brain.
Whether or not glymphatic disruption has a role to play as a risk factor for migraine isn’t yet known, but the findings could bring us closer to more effective therapies for the management of migraines.
“The results of our study could help inspire future, larger-scale studies to continue investigating how changes in the brain’s microscopic vessels and blood supply contribute to different migraine types,” Xu concluded. “Eventually, this could help us develop new, personalized ways to diagnose and treat migraine.”
The findings will be presented at the annual meeting of the Radiological Society of North America.