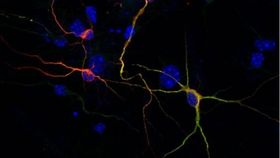
The ability to give cells new identities in the lab holds huge potential not just to dramatically improve our knowledge of cell biology and disease, but also for the promising fields of regenerative and personalized medicine. And scientists may have just made a giant stride in this area, as two groups in China have independently come up with techniques that allow for the conversion of skin cells into neurons, without the need to introduce potentially problematic genes.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.Using a cocktail of small molecules, the researchers demonstrated it was possible to convert skin cells from humans, including Alzheimer’s patients, and mice into brain cells. Not only did the cells take on the appearance of normal neurons and those converted by other means, they also functioned like the real thing, even firing and forming connections with one another. Both studies have been published in Cell Stem Cell.
Scientists have been able to induce cellular identity swaps in the lab for some time now, but usually this involves manipulating which genes are switched on or off using proteins called transcription factors. By targeting those specific to a certain cell type, it is possible to essentially turn back the clock and coax the cells into assuming a more blank slate state, or pluripotent state. Scientists can then manipulate their environment and direct their fate into a cell of desire.
While an extremely useful technique, its potential therapeutic applications have been limited by the fact that it often necessitates the introduction of transgenes, which carries a cancer risk should they end up in an off-target location and switch on genes that can cause cell replication to go awry. Using small chemical molecules to achieve the same outcome, however, attempts to overcome this issue and offers numerous advantages.
Namely, avoiding genetic manipulation and the need to pass through a stem cell phase reduces some safety concerns, and because the molecules can slide through the cell’s membranes to reach the DNA, they don’t require the use of viruses for delivery. Furthermore, they’re cheaper, easy to synthesize and produce reversible effects.
The first of the two studies to probe the potential of these molecules involved adding a chemical cocktail to skin cells derived from healthy patients and individuals with Alzheimer’s. By adding them in two different stages, the researchers were able to dampen skin cell-specific genes and then drive expression of native neuronal transcription factors. In just a few weeks, the cells assumed a new neuronal identity, looking and behaving like neurons produced using the transgenic approach.
In the second, researchers achieved the same feat with mouse skin cells, but using a different combination of small molecules. Impressively, in just 16 days, 90% of the initial cell population was positive for a neuron-specific protein called TUJ1. Furthermore, the cells could generate action potentials that are critical to neuronal firing, and they formed functional junctions with one another across which information can be transmitted.
While the researchers need to fine-tune the processes, the proof-of-concept work is certainly encouraging. If researchers are able to generate personalized batches of cells, it may be possible to graft them into patients as a means of disease treatment. Furthermore, using patients who already suffer neurological diseases, such as Alzheimer’s, researchers may be able to learn more about these conditions by studying their cells in the lab.