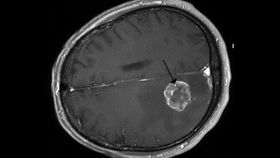
The blood-brain barrier (BBB) is just as it sounds: an incredibly selective permeable membrane that separates blood from the brain. While this does a great job of keeping the brain healthy and preventing contaminants in the blood from affecting the brain, it also makes it more difficult to use medications to target neurological disorders. Only a few types of drugs can make it through, and they usually come with a host of nasty side effects. However, a group of researchers are about to begin clinical trials on a technique that uses MRI-guided ultrasound to open up the BBB in order to give access to drugs that could treat diseases like cancer, Alzheimer’s, and Parkinson’s. The research will use 10 patients who have been diagnosed with cancerous brain tumors.
The rest of this article is behind a paywall. Please sign in or subscribe to access the full content.A paper from researchers at Harvard Medical School was published in PLOS ONE back in 2012, demonstrating the success of the technique using four rhesus macaques. Over the course of 22 weekly sessions, the team had a 96% success rate of disrupting the BBB. The success was measured by the presence of MRI contrast agent in the brain, which is normally not able to pass the BBB. There were no adverse consequences for the animals used in the study, and the researchers noted the results were “promising for clinical translation of this technology.”
The human trial will involve multiple steps. First, chemotherapy medication will be introduced to the bloodstream. Next, the patient an injection of microbubbles that will be carried around the body, including to the capillaries near the BBB. Then, highly targeted ultrasound waves will send pulses toward the tumor. This will cause the microbubbles to vibrate about 200,000 times per second, wriggling open a wider passage through the BBB. It is hoped that this will be enough for the chemo to pass through and begin to treat the tumor. Fluorescent markers will be attached to the drugs in order to track their location.
The entire process doesn’t last very long, as nine different sites around the tumor can be opened after two minutes of exposure to the ultrasound. As soon as the ultrasound is turned off, the BBB will begin to close over the next 6 hours. Though this does put the brain temporarily at risk of being contaminated by bacteria in the blood, the risk isn’t any greater than when surgery is performed on the brain.
What isn’t known, however, is how well the drugs will move through the brain once they pass the BBB. For diseases that affect a large portion of the brain, such as Alzheimer’s, the patient would likely have to undergo multiple sessions in order to treat the entire brain. Testing in animals has shown that disruption of the BBB for an entire hemisphere be done without any longterm adverse affects.
Currently, there aren’t many great options for treating Alzheimer’s. There are four FDA-approved cholinesterase inhibitors that slow disease as well as one drug that blocks NMDA receptors, slowing cell damage. These treatments only work for about half of the people with the disease, and the drugs typically only work for 6-12 months. Disrupting the BBB opens the door to new medications. For instance, there are antibody treatments which do a fantastic job of clearing plaques from brain tissue in vitro, but isn’t able to cross the BBB to work as an effective treatment within the brain.
It will still be several years before this method is a viable clinical option, but the fact that it is moving to human trials is incredibly exciting. With any luck, the burgeoning field of nanomedicine will couple with this unprecedented amount of access to the brain, bringing effective treatment of those with brain tumors, Alzheimer’s, depression, Parkinson’s, and scores of other disorders.
[Hat tip: Helen Thompson, New Scientist]